February 11, 2025February 24, 2026
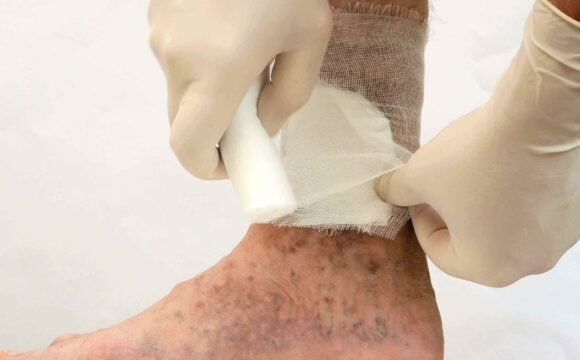
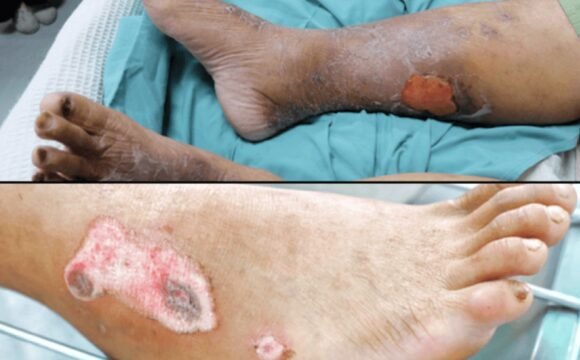
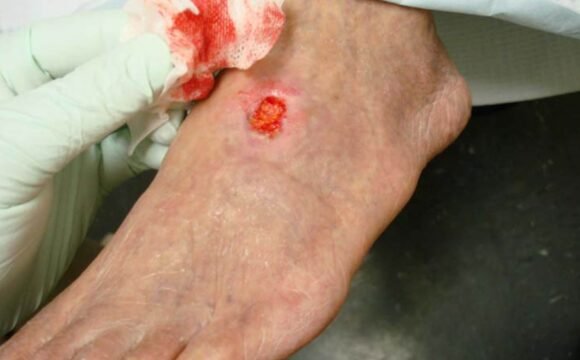
Arterial Ulcers
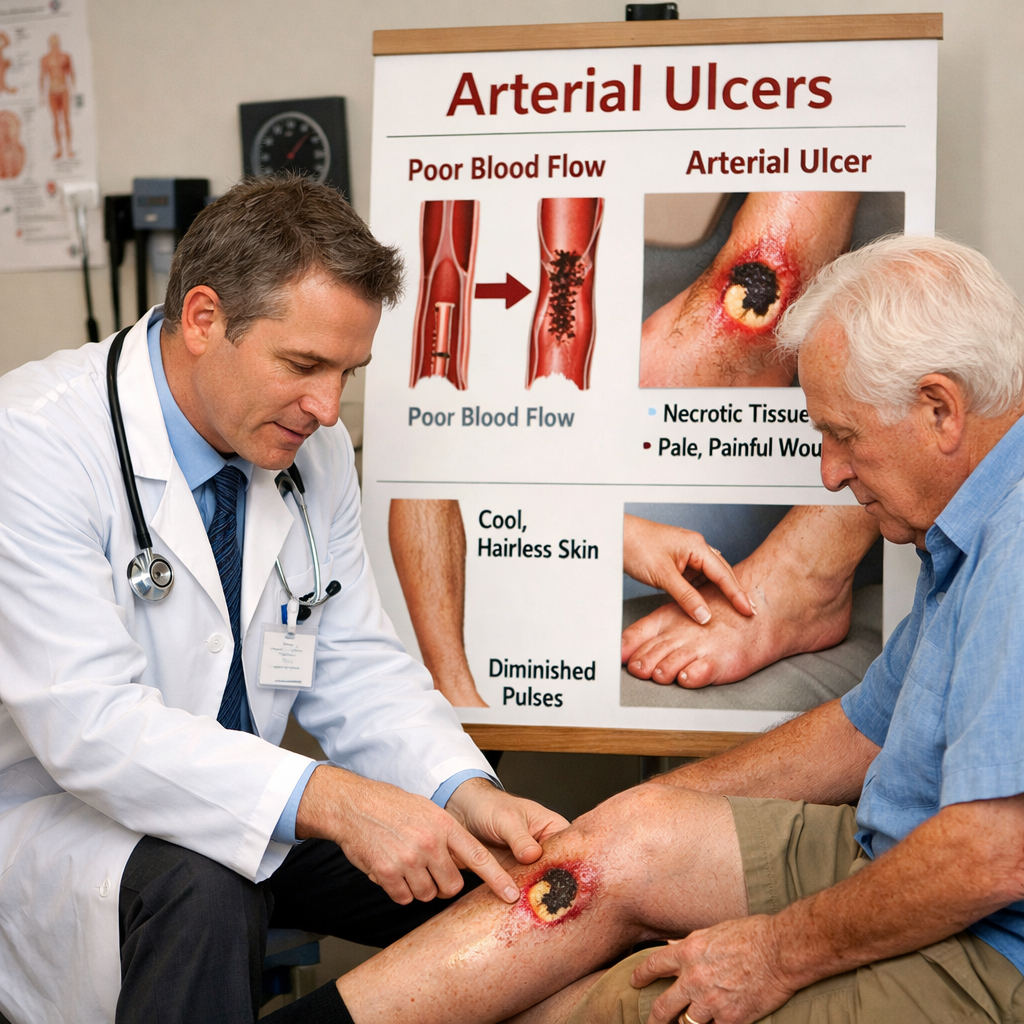
Arterial Ulcers Demystified: Causes, Treatment, and Healing Tips You Need
Arterial ulcers, also known as ischemic ulcers, are one of the most challenging types of wounds to manage. These ulcers are often painful, slow to heal, and a sign of underlying arterial disease. If left untreated, they can lead to severe complications, including infections and, in extreme cases, limb amputation. Understanding arterial ulcers, their causes, types, and effective treatment strategies is crucial not only for healthcare professionals but also for patients and caregivers.
In this comprehensive guide, we will explore arterial ulcers in depth, from their causes to their healing process, and provide practical wound care guidance for better outcomes.
What Are Arterial Ulcers?
Arterial ulcers are wounds that occur due to poor blood circulation in the arteries. The arteries are responsible for delivering oxygen-rich blood to tissues. When they become narrowed or blocked, tissues may not get enough oxygen, resulting in tissue death and the formation of ulcers.
These ulcers most commonly occur on the lower legs, feet, toes, and heels—areas farthest from the heart where blood circulation is already more vulnerable. Unlike other wounds, arterial ulcers are typically painful, deep, and slow to heal.
Causes of Arterial Ulcers
Arterial ulcers are primarily caused by peripheral artery disease (PAD), but other factors can contribute. Here are the main causes:
- Atherosclerosis (Hardening of the Arteries): This is the most common cause. Plaque builds up inside arteries, reducing blood flow to the limbs.
- Diabetes: High blood sugar levels can damage blood vessels and nerves, making arterial ulcers more likely.
- Hypertension (High Blood Pressure): Persistent high blood pressure can weaken arteries, reducing circulation.
- Smoking: Nicotine constricts blood vessels, further limiting blood supply to the extremities.
- Cholesterol and Lipid Disorders: Elevated cholesterol can accelerate plaque buildup in arteries.
- Aging: Older adults are more prone to arterial narrowing and ulcers.
- Trauma or Pressure: Even minor injuries can become problematic when blood flow is restricted, leading to slow-healing ulcers.
Types of Arterial Ulcers
Arterial ulcers can be classified based on location, appearance, and underlying pathology. Understanding the type helps guide treatment.
1. Ischemic Ulcers
- Location: Usually on the toes, heels, or pressure points.
- Appearance: Deep, pale, and often with a punched-out look.
- Symptoms: Severe pain, especially at night or when legs are elevated.
2. Gangrenous Ulcers
- Location: Typically on toes or feet.
- Appearance: Black or dark brown tissue (necrosis) due to extreme lack of blood flow.
- Symptoms: Severe pain initially, followed by numbness as tissue dies.
3. Necrotic Ulcers
- Location: Anywhere on the lower limb.
- Appearance: Dead tissue that is black, gray, or yellow.
- Symptoms: Often associated with infection risk.
4. Toe and Heel Ulcers
- Location: Toes and heels are common due to minimal padding and blood supply.
- Appearance: Small but extremely painful.
- Symptoms: Pain increases when legs are elevated.
5. Multiple Arterial Ulcers
- Location: May appear on different toes or both feet.
- Appearance: Varying sizes; usually deep with well-defined edges.
- Symptoms: Painful, with delayed healing.
Symptoms and Signs of Arterial Ulcers
Recognizing arterial ulcers early can prevent complications. Key signs include:
- Severe pain, particularly at night or when legs are elevated
- Small, round, deep ulcers with well-defined borders
- Pale, shiny, and thin skin around the ulcer
- Cool or cold feet due to poor circulation
- Weak or absent pulses in the affected limb
- Delayed healing and recurrent wounds
Unlike venous ulcers, arterial ulcers are often painful rather than itchy and are not typically accompanied by swelling.
Diagnosis of Arterial Ulcers
Healthcare providers use multiple methods to diagnose arterial ulcers:
- Physical Examination: Inspecting the ulcer, checking skin temperature, and feeling pulses.
- Ankle-Brachial Index (ABI): A simple test comparing blood pressure in the ankle to the arm. An ABI < 0.9 indicates poor arterial circulation.
- Doppler Ultrasound: Evaluates blood flow in the arteries.
- Angiography: Imaging that shows arterial blockages and narrowing.
- Laboratory Tests: Blood sugar, cholesterol, and infection markers may be assessed.
Treatment of Arterial Ulcers
Treating arterial ulcers involves addressing both the ulcer itself and the underlying arterial disease. Effective management often requires a multidisciplinary approach.
1. Improving Blood Circulation
- Medications: Blood thinners, antiplatelet drugs, and vasodilators may be prescribed.
- Surgery: Procedures like angioplasty or bypass surgery can restore blood flow.
2. Wound Care and Dressing
Proper wound care is essential for healing:
- Cleaning the wound: Use sterile saline to remove debris.
- Debridement: Removal of dead tissue to encourage healing.
- Dressing selection: Non-adherent or hydrocolloid dressings help maintain a moist healing environment.
- Monitoring infection: Antibiotics may be used if infection is present.
3. Pain Management
Pain can be severe in arterial ulcers. Management strategies include:
- Over-the-counter painkillers (acetaminophen, ibuprofen)
- Prescription medications for severe pain
- Elevating the legs minimally; excessive elevation can worsen pain
4. Lifestyle Modifications
- Quit smoking: Essential for improving circulation
- Control diabetes: Maintain blood sugar within target range
- Exercise: Gentle, supervised exercises improve circulation
5. Preventing Recurrence
- Wear protective footwear to avoid trauma
- Inspect feet daily for early signs of ulcers
- Maintain a healthy diet to reduce arterial plaque
The Healing Process of Arterial Ulcers
Arterial ulcers are slow to heal because they occur in areas with poor blood supply. The healing process can be broken down into stages:
- Inflammatory Phase
- The body responds to tissue damage with swelling, redness, and pain.
- White blood cells work to prevent infection.
- Proliferative Phase
- New tissue forms, including collagen and blood vessels.
- Growth of granulation tissue is crucial for filling the ulcer.
- Maturation Phase
- Collagen reorganizes, and the wound contracts.
- Healing is often incomplete without improving blood flow.
Healing can take weeks to months, depending on ulcer size, circulation, and overall health.
Wound Care Guide for Arterial Ulcers
Here’s a practical guide for caring for arterial ulcers at home or in a clinical setting:
Step 1: Assess the Wound
- Check size, depth, and surrounding skin
- Note any odor, drainage, or signs of infection
Step 2: Clean the Wound
- Use sterile saline or prescribed wound cleanser
- Avoid harsh antiseptics that damage healthy tissue
Step 3: Debride Dead Tissue
- Remove necrotic tissue carefully, preferably under professional supervision
Step 4: Apply Appropriate Dressing
- Hydrocolloid, foam, or alginate dressings keep the wound moist
- Change dressing as recommended by a healthcare provider
Step 5: Monitor for Infection
- Redness, warmth, pus, or foul odor are warning signs
- Seek medical attention immediately if infection is suspected
Step 6: Optimize Circulation
- Avoid excessive leg elevation
- Gentle exercises or physiotherapy may help
Step 7: Follow-Up Care
- Regular check-ups with a vascular specialist
- Adjust treatment based on healing progress
Complications of Arterial Ulcers
If left untreated, arterial ulcers can lead to serious complications:
- Infections: Can spread to deeper tissues (cellulitis or osteomyelitis)
- Gangrene: Tissue death may require amputation
- Chronic pain: Persistent discomfort affecting quality of life
- Delayed healing: Often worsened by diabetes or smoking
Prevention of Arterial Ulcers
Preventing arterial ulcers focuses on maintaining healthy circulation and protecting the feet:
- Quit smoking and control blood sugar
- Maintain a healthy diet and exercise regularly
- Inspect feet daily for injuries or skin changes
- Wear well-fitting shoes and avoid walking barefoot
- Manage blood pressure and cholesterol
When to Seek Medical Help
Seek immediate attention if you notice:
- Severe pain that does not improve
- Wound that is enlarging or not healing
- Signs of infection (redness, pus, swelling)
- Black or dark tissue on toes or feet
Early intervention can save limbs and prevent serious complications.
Conclusion
Arterial ulcers are more than just wounds they are a sign of underlying vascular disease that requires careful attention. With proper care, lifestyle changes, and medical intervention, healing is possible, and recurrence can be minimized.
By understanding causes, types, treatment, and the healing process, patients and caregivers can take proactive steps to manage arterial ulcers effectively. Remember, timely medical care and consistent wound management are the keys to successful recovery.