February 02, 2026February 25, 2026
Diabetic Foot Ulcers
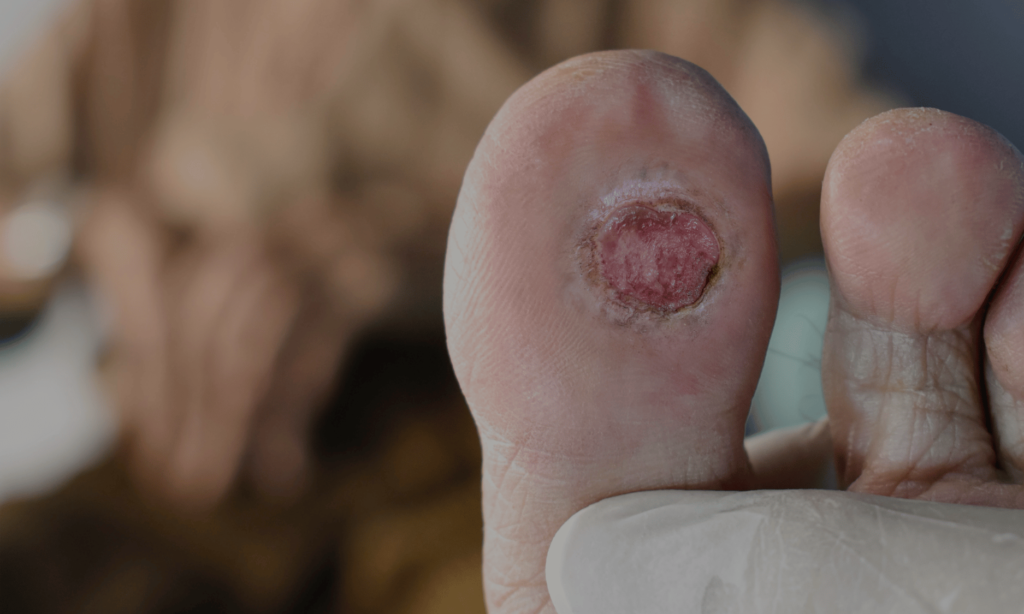
Diabetic Foot Ulcer: Complete Wound Guide for Prevention, Care & Healing
A diabetic foot ulcer is one of the most serious complications of diabetes. It develops when high blood sugar damages nerves and blood vessels, making even a small cut or blister turn into a deep, non-healing wound. If not treated early, these ulcers can lead to severe infections and even amputation.
This detailed wound guide will help you understand what diabetic foot ulcers are, why they happen, and how proper care can support faster healing and prevent complications.
What Is a Diabetic Foot Ulcer?
A diabetic foot ulcer is an open sore or wound that usually appears on the bottom of the foot. It occurs due to a combination of nerve damage (neuropathy), poor circulation, and pressure on certain areas of the foot.
People with diabetes may not feel pain from minor injuries because nerve damage reduces sensation. As a result, wounds may worsen without being noticed.
Common Causes of Diabetic Foot Ulcer
1. Peripheral Neuropathy
Nerve damage reduces the ability to feel pain or pressure, increasing injury risk.
2. Poor Blood Circulation
Reduced blood flow slows the healing process and raises infection risk.
3. High Blood Sugar Levels
Uncontrolled diabetes weakens immunity and damages tissues.
4. Foot Deformities or Pressure Points
Bunions, calluses, or improper footwear can create constant friction.
5. Infection
Even small cuts can become infected quickly in diabetic patients.
Signs and Symptoms to Watch
Early detection is extremely important. Look for:
- Redness or swelling on the foot
- Open sores that don’t heal
- Drainage or pus
- Bad odor from the wound
- Warm skin around the area
- Black tissue (possible tissue death)
If you notice any of these signs, follow a proper wound guide and seek medical advice immediately.
Risk Factors That Increase Chances
Some people are more likely to develop diabetic foot ulcers, especially those who:
- Have had diabetes for many years
- Smoke or use tobacco
- Have poor blood sugar control
- Walk barefoot frequently
- Have previous foot injuries
- Are overweight or less physically active
Understanding these risks helps in creating a strong prevention strategy.
Diagnosis and Medical Assessment
Doctors evaluate diabetic foot ulcers using different methods:
- Physical examination of the wound
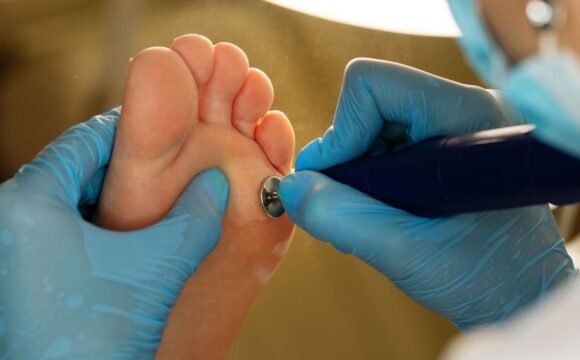
- Checking foot sensation with monofilament testing
- Blood circulation assessment
- Imaging tests if bone infection is suspected
- Blood tests to monitor sugar levels and infection
Accurate diagnosis helps create a personalized wound guide tailored to the patient’s condition.
Treatment Options for Diabetic Foot Ulcer
1. Wound Cleaning and Debridement
Removing dead tissue allows healthy skin to grow.
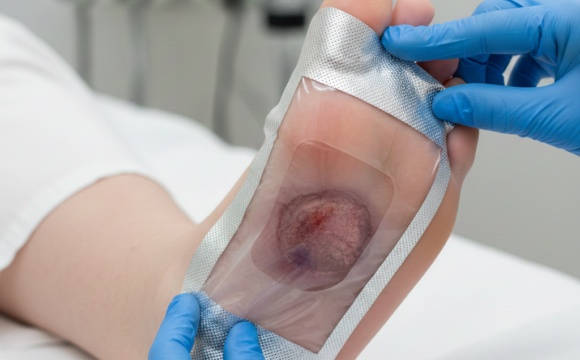
2. Advanced Wound Dressings
Moisture-balanced dressings protect the wound and support healing.
3. Infection Control
Antibiotics may be prescribed when infection is present.
4. Offloading Pressure
Special shoes, casts, or orthotic devices reduce pressure on the ulcer.
5. Blood Sugar Management
Stable glucose levels are essential for faster healing.
6. Surgical Treatment (When Needed)
Severe ulcers may require procedures such as skin grafting or vascular surgery
Advanced Therapies Used Today
Modern treatments can improve outcomes for difficult wounds:
- Negative pressure wound therapy
- Hyperbaric oxygen therapy
- Growth factor therapy
- Bioengineered skin substitutes
These therapies are often recommended as part of an advanced wound guide when standard care isn’t enough.
Daily Foot Care: Essential Wound Guide for Patients
Consistent foot care can prevent ulcers and help existing wounds heal faster:
- Check your feet daily for cuts or redness
- Wash with lukewarm water and dry gently
- Moisturize dry skin (avoid between toes)
- Trim nails carefully
- Wear soft, well-fitted shoes
- Never walk barefoot
Small habits make a big difference in preventing complications.
Role of Nutrition in Healing
Nutrition plays a major role in tissue repair. Patients should include:
- High-protein foods for tissue rebuilding
- Vitamin C for collagen formation
- Zinc for immune support
- Adequate hydration
A balanced diet is a key element in any effective wound guide for diabetic patients.
Prevention Tips for Diabetic Foot Ulcers
Prevention focuses on controlling diabetes and protecting the feet.
- Maintain healthy blood sugar levels
- Stop smoking
- Exercise regularly to improve circulation
- Schedule routine foot checkups
- Use diabetic-friendly footwear
- Treat small cuts immediately
Early action reduces the risk of chronic non-healing wounds.
Emotional and Lifestyle Impact
Living with a diabetic foot ulcer can affect daily life and mental health. Pain, mobility issues, and fear of complications can cause stress. Education through reliable resources like Wound Guide helps patients feel more confident and informed throughout their healing journey.
When Should You Seek Immediate Medical Help?
Consult a healthcare professional if:
- The wound becomes deeper or larger
- Fever or severe pain develops
- The skin turns black or blue
- There is heavy drainage or odor
Prompt treatment prevents serious complications.
Conclusion: Your Complete Wound Guide for Diabetic Foot Ulcer Care
A diabetic foot ulcer is serious but manageable with the right care and early intervention. Understanding risk factors, maintaining proper hygiene, controlling blood sugar, and following a structured wound guide can significantly improve healing outcomes.
By staying informed and proactive with support from trusted resources like Wound Guide patients can protect their feet, reduce complications, and move toward a healthier, more active life.