August 20, 2025February 24, 2026
Pressure Ulcers (Bedsores)
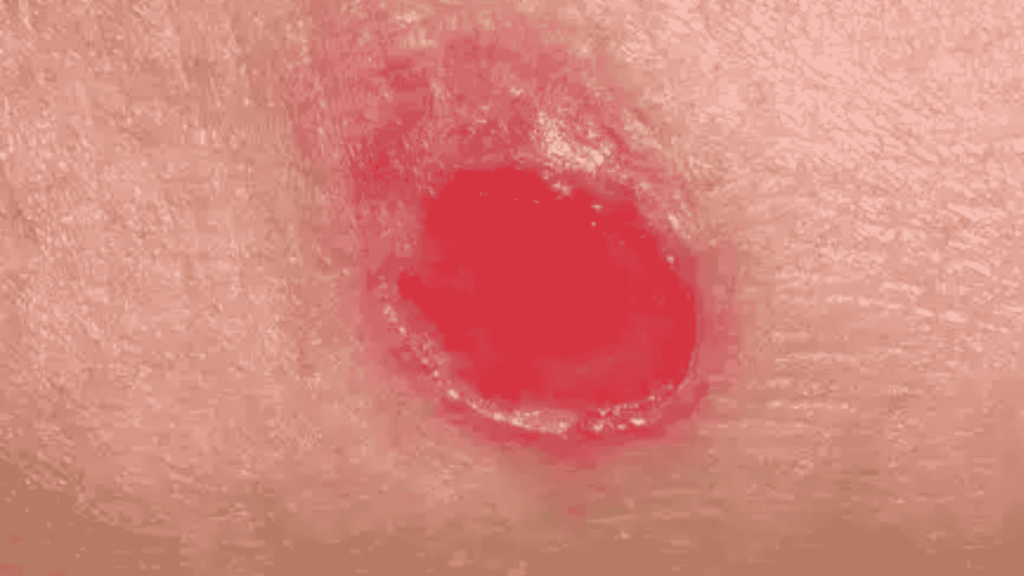
Pressure Ulcers: Complete Wound Guide for Prevention, Stages & Faster Healing
Pressure ulcers, also known as bedsores, are injuries to the skin and underlying tissue caused by prolonged pressure on certain parts of the body. They commonly develop in individuals who spend long periods in bed or in a wheelchair, especially elderly patients or those with limited mobility. Without proper care, pressure ulcers can worsen quickly, leading to infection, pain, and serious health complications.
This detailed Wound Guide will help you understand the causes, stages, symptoms, treatment options, and prevention strategies for pressure ulcers so patients and caregivers can support safer and faster healing.
What Are Pressure Ulcers?
Pressure ulcers occur when constant pressure reduces blood flow to the skin. When tissues do not receive enough oxygen and nutrients, they begin to break down, forming sores.
Common areas where pressure ulcers develop include:
- Heels
- Ankles
- Hips
- Tailbone (sacrum)
- Elbows
- Shoulder blades
- Back of the head
These wounds can range from mild skin redness to deep injuries affecting muscles and bones.
Why Do Pressure Ulcers Develop?
Pressure ulcers are often caused by a combination of pressure, friction, and moisture. Understanding the main causes helps caregivers follow a proper wound guide.
1. Prolonged Pressure
Remaining in the same position for too long reduces blood circulation.
2. Friction and Shear
Sliding across bed sheets can damage fragile skin layers.
3. Moisture
Sweat, urine, or wound drainage weakens skin integrity.
4. Poor Nutrition
Lack of protein and vitamins slows tissue repair.
5. Medical Conditions
Diabetes, vascular disease, and spinal injuries increase risk.
Stages of Pressure Ulcers
Pressure ulcers are classified into stages based on severity. Identifying the stage helps guide treatment.
Stage 1: Early Skin Damage
- Redness that does not fade
- Skin may feel warm or firm
- No open wound yet
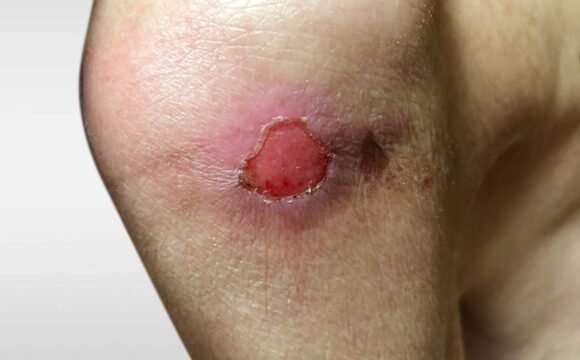
Stage 2: Partial Skin Loss
- Shallow open sore or blister
- Pain and tenderness
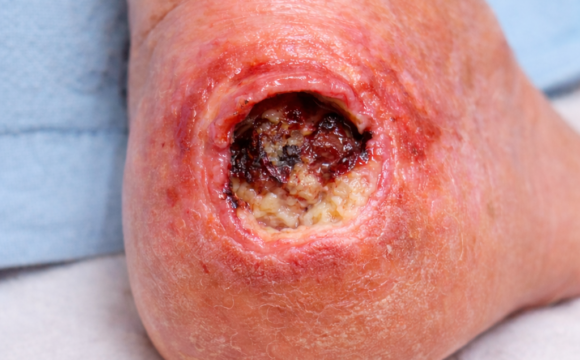
Stage 3: Deep Tissue Damage
- Wound extends into fat tissue
- Possible drainage and odor
Stage 4: Severe Ulcer
- Exposure of muscle or bone
- High infection risk
Following a structured Wound Guide during early stages can prevent progression to severe wounds.
Signs and Symptoms to Watch
Caregivers should monitor skin daily for early warning signs:
- Persistent redness or discoloration
- Swelling or warmth
- Pain or itching
- Open sores
- Drainage or foul odor
Early detection is one of the most effective ways to prevent complications.
Who Is at High Risk?
Certain individuals are more vulnerable to pressure ulcers:
- Bedridden or wheelchair-bound patients
- Elderly individuals
- Patients with spinal cord injuries
- People with poor circulation
- Individuals with diabetes
- Those with limited mobility after surgery
Regular repositioning and following a professional wound guide are essential for these high-risk groups.
Diagnosis and Medical Assessment
Healthcare professionals assess pressure ulcers using:
- Visual examination of the skin
- Measuring wound size and depth
- Checking for infection signs
- Nutritional evaluation
- Blood circulation tests
Proper assessment ensures that treatment addresses both the wound and underlying health issues.
Treatment Options for Pressure Ulcers
Treatment depends on the stage and severity of the ulcer.
1. Pressure Relief and Repositioning
Changing body position every two hours reduces pressure buildup.
2. Wound Cleaning and Debridement
Removing dead tissue helps healthy skin grow.
3. Advanced Dressings
Hydrocolloid, foam, or antimicrobial dressings maintain moisture balance.
4. Infection Control
Antibiotics may be needed if bacteria are present.
5. Support Surfaces
Special mattresses and cushions reduce pressure on vulnerable areas.
A personalized Wound Guide ensures consistency in care and faster healing.
Advanced Therapies for Severe Pressure Ulcers
Modern wound care technologies provide additional support for complex wounds:
- Negative pressure wound therapy
- Electrical stimulation therapy
- Hyperbaric oxygen therapy
- Bioengineered skin substitutes
These treatments are often used when traditional care does not achieve desired results.
Daily Care Tips: Practical Wound Guide for Caregivers
Proper daily care is essential for managing pressure ulcers effectively:
- Reposition the patient regularly
- Keep skin clean and dry
- Use gentle cleansing products
- Inspect skin daily for redness or breakdown
- Apply moisturizers to prevent dryness
- Use pressure-relieving cushions or mattresses
Consistent care can prevent new ulcers from forming.
Role of Nutrition in Pressure Ulcer Healing
Nutrition plays a key role in tissue repair and immune strength.
Important nutrients include:
- Protein: Supports skin rebuilding
- Vitamin C: Promotes collagen production
- Zinc: Enhances healing response
- Hydration: Maintains skin elasticity
A balanced diet is a core component of any effective Wound Guide for pressure ulcer management.
Preventing Pressure Ulcers
Prevention is always easier than treatment. Follow these essential tips:
- Change positions frequently
- Use supportive bedding
- Maintain healthy skin hygiene
- Encourage movement and physical activity
- Monitor weight and nutrition
- Manage chronic health conditions
Education and awareness through platforms like Wound Guide help caregivers prevent pressure ulcers before they become serious.
Emotional and Lifestyle Impact
Living with pressure ulcers can be physically uncomfortable and emotionally challenging. Patients may experience reduced mobility, sleep disturbances, and frustration during long healing periods. Support from caregivers and access to reliable educational resources like Wound Guide can improve confidence and quality of life.
When Should You Seek Medical Help?
Contact a healthcare professional immediately if:
- The wound becomes deeper or darker
- Fever or infection symptoms develop
- There is heavy drainage or odor
- Pain suddenly increases
- Surrounding skin turns black or purple
Early treatment reduces complications and improves recovery outcomes.
Future of Pressure Ulcer Care
Advancements in medical technology are improving how pressure ulcers are managed. Smart dressings, AI-based wound monitoring, and regenerative therapies are helping healthcare providers detect problems earlier and support faster healing. Educational resources like Wound Guide continue to play a vital role in spreading awareness and improving patient care.
Conclusion: Your Complete Wound Guide for Pressure Ulcers
Pressure ulcers can be serious, but they are largely preventable with proper care and awareness. Understanding the stages, recognizing early symptoms, and following a structured Wound Guide can make a significant difference in healing outcomes.
Regular repositioning, proper nutrition, advanced wound care techniques, and support from trusted resources like Wound Guide empower patients and caregivers to manage pressure ulcers effectively and improve overall well-being.