February 12, 2025February 24, 2026
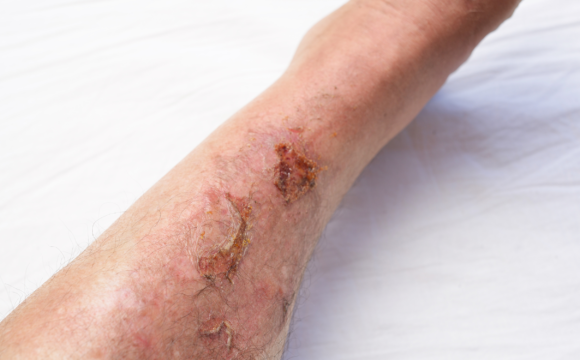
Chronic Non-Healing Wounds
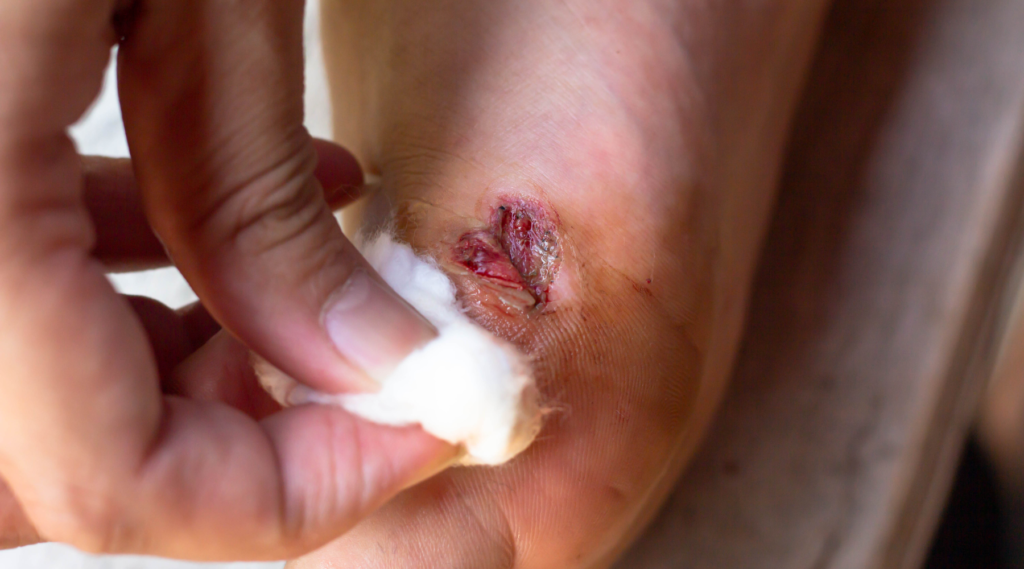
Chronic Non-Healing Wounds: Complete Wound Guide for Better Healing
Chronic non-healing wounds are a growing healthcare concern worldwide. Unlike normal injuries that heal within weeks, these wounds remain open for months and sometimes even years. They can cause pain, infections, emotional stress, and serious health complications if not treated properly. Understanding why wounds fail to heal and how to manage them effectively is the first step toward recovery.
This detailed wound guide will help you understand the causes, risk factors, treatment strategies, and preventive care for chronic non-healing wounds so you or your patients can achieve faster and safer healing.
What Are Chronic Non-Healing Wounds?
A chronic wound is any wound that does not progress through the normal stages of healing within about 4 to 6 weeks. These wounds often remain inflamed, infected, or poorly supplied with blood, making recovery slow and complicated.
Common types of chronic non-healing wounds include:
- Diabetic foot ulcers
- Pressure ulcers (bedsores)
- Venous leg ulcers
- Arterial ulcers
- Surgical wounds that fail to heal
Normally, wound healing happens in four stages: hemostasis, inflammation, proliferation, and remodeling. When one of these stages gets disrupted, the wound becomes chronic.
Why Do Some Wounds Become Chronic?
Many factors can prevent proper healing. The body needs good circulation, proper nutrition, and a strong immune response to repair damaged tissue. When these conditions are not met, wounds may stay open longer.
1. Poor Blood Circulation
Reduced blood flow means less oxygen and nutrients reach the wound, slowing tissue repair.
2. Diabetes
High blood sugar damages nerves and blood vessels, making diabetic patients highly prone to chronic wounds.
3. Infection
Bacteria in the wound increase inflammation and prevent new tissue formation.
4. Repeated Pressure or Trauma
Constant pressure on certain body parts — especially in bedridden patients — stops wounds from healing.
5. Weak Immune System
Chronic illnesses or certain medications can reduce the body’s ability to fight infection and regenerate tissue.
Signs and Symptoms of Chronic Non-Healing Wounds
Recognizing early warning signs can prevent serious complications. Watch for:
- Wound lasting more than 4 weeks
- Persistent redness or swelling
- Unpleasant odor or discharge
- Increasing pain
- Black or dead tissue around the wound
- Fever or general weakness
If any of these symptoms appear, medical attention is essential. Early diagnosis plays a huge role in successful wound care.
Risk Factors You Should Know
Certain lifestyle and health conditions increase the risk of chronic wounds:
- Diabetes or uncontrolled blood sugar
- Smoking
- Obesity
- Poor nutrition
- Advanced age
- Limited mobility
- Vascular disease
Following a structured wound guide and improving daily habits can significantly reduce these risks.
Diagnosis and Assessment
Healthcare professionals use multiple methods to evaluate chronic wounds. A proper assessment helps identify the root cause and decide the right treatment plan.
Common diagnostic steps include:
- Measuring wound size and depth
- Checking blood circulation
- Infection testing
- Imaging tests if bone involvement is suspected
- Blood sugar monitoring in diabetic patients
Regular assessment ensures that the wound care strategy stays effective.
Effective Treatment Options for Chronic Non-Healing Wounds
Treatment depends on the cause, severity, and overall health of the patient. A personalized wound guide often includes multiple therapies.
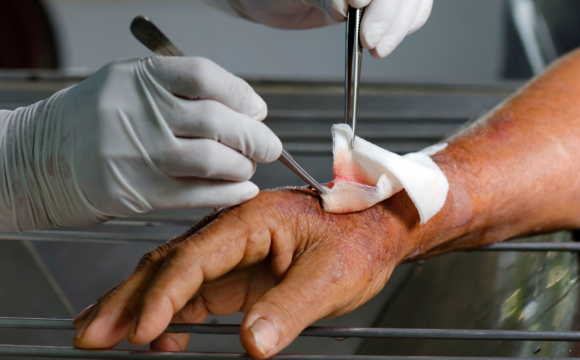
1. Proper Wound Cleaning and Debridement
Removing dead tissue encourages healthy tissue growth and reduces infection risk.
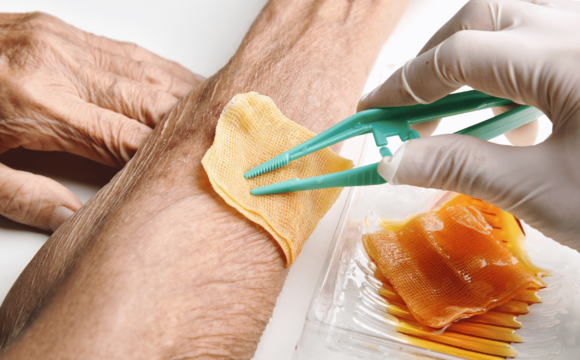
2. Advanced Dressings
Modern wound dressings maintain moisture balance, protect from bacteria, and promote faster healing.
3. Infection Control
Antibiotics or antimicrobial dressings may be required if infection is present.
4. Pressure Offloading
Special footwear or cushions reduce pressure on wounds, especially in diabetic foot ulcers.
5. Blood Sugar Management
For diabetic patients, stable glucose levels are essential for recovery.
6. Nutritional Support
Protein, vitamins C and A, zinc, and hydration help tissue regeneration.
Advanced Therapies for Faster Healing
Modern medicine offers several innovative options for difficult wounds:
- Negative pressure wound therapy (vacuum therapy)
- Skin grafting
- Growth factor therapy
- Hyperbaric oxygen therapy
- Bioengineered skin substitutes
These treatments are often included in a professional wound guide when standard methods are not enough.
Home Care Tips: Daily Wound Guide for Patients
Managing chronic wounds at home requires consistency and hygiene. Here are practical steps:
- Wash hands before touching the wound
- Follow dressing change instructions carefully
- Keep the wound clean and dry
- Avoid smoking and alcohol
- Maintain a balanced diet
- Monitor for signs of infection
Patients should never ignore changes in wound appearance or sudden pain.
The Role of Nutrition in Healing
Nutrition is one of the most overlooked aspects of chronic wound care. Without proper nutrients, the body cannot rebuild damaged tissue.
Key nutrients include:
- Protein: Supports tissue repair
- Vitamin C: Helps collagen production
- Zinc: Boosts immune function
- Iron: Improves oxygen delivery
A well-structured diet plan is an important part of any effective wound guide.
Preventing Chronic Non-Healing Wounds
Prevention is always better than treatment. Small lifestyle changes can significantly reduce the risk.
Maintain Healthy Blood Sugar
Regular monitoring and proper medication help prevent diabetic ulcers.
Stay Active
Movement improves blood circulation and reduces pressure sores.
Check Feet Daily
Especially important for diabetic patients.
Use Proper Footwear
Supportive shoes prevent injuries that may become chronic wounds.
Follow Regular Medical Checkups
Early intervention can stop minor wounds from becoming serious.
Emotional Impact of Chronic Wounds
Living with a long-term wound can affect mental health. Pain, limited mobility, and slow recovery may lead to stress or anxiety. Support from family, caregivers, and healthcare professionals is essential.
Educational platforms like Wound Guide help patients understand their condition, making them feel more confident and informed throughout their healing journey.
When Should You See a Specialist?
Seek medical advice immediately if:
- The wound grows larger
- There is severe pain or swelling
- Fever or infection symptoms appear
- The wound turns black or has foul discharge
Early professional care can prevent complications such as amputation or systemic infection.
Future of Chronic Wound Care
The future of wound care is evolving rapidly. Researchers are developing smart dressings, AI-based wound monitoring, and regenerative therapies to improve healing outcomes.
Digital platforms and educational resources like Wound Guide are also helping patients access reliable information and better treatment options.
Conclusion: A Complete Wound Guide for Better Healing
Chronic non-healing wounds require patience, proper treatment, and a well-structured care plan. Understanding the root causes, recognizing early symptoms, and following the right wound guide can significantly improve healing outcomes.
Whether caused by diabetes, pressure, or poor circulation, these wounds should never be ignored. With advanced therapies, proper nutrition, and consistent care, recovery is possible. Education and awareness supported by reliable resources like Wound Guide empower patients to take control of their healing journey and move toward a healthier future.